the PEO Platform for
reconciliation and EDI
10+ years helping the leading PEOs stop premium leakage and deliver EDI files.
Works with any HRIS, Payroll, or COBRA systems
Trusted By:

How Our PEO
SOFTWARE HELPS
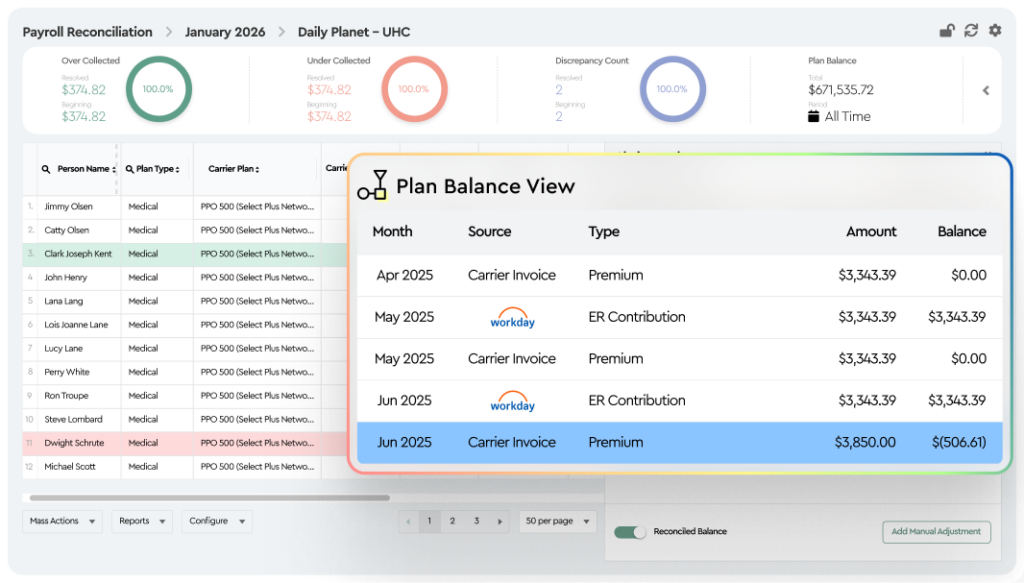
Benefits Reconciliation for PEOs
Catch premium
variances faster
Replace spreadsheets with automated matching of carrier invoices against enrollment and payroll data.
EDI Connectivity for PEOs
Deliver EDI Files
in 30-Days
From enrollment data to carrier-ready 834 files – Tabulera handles the entire EDI pipeline for your PEO.

Tabulera’s Benefits reconciliation
Equip your PEO with a platform that replaces the spreadsheet – a structured workflow your team can follow to reconcile faster.

Automated Matching
Upload invoices. Tabulera does the rest.
- Auto-Matches against HRIS, Payroll and COBRA
- Auto-resolves timing differences
- Surfaces only real exceptions
Variance Tracking
Every discrepancy tracked until closed.
- Open items visible until resolved
- Follow-ups and notes logged
- Complete audit trail for every resolution

Reconciliation Reporting
Every cycle documented and shareable.
- Totals, adjustments, and costs per employee
- Export to Excel in one click
- Audit-ready for finance, carriers, or clients
Why PEOs Still Reconcile Benefits in Spreadsheets
Payroll? Covered. Enrollment? Covered. Reconciliation? Still a spreadsheet. One person owns it. Everyone depends on it. Nobody talks about what happens if that person leaves.
We analyzed 11,674 premium invoices. Here's what we found.
92% of all line records lined up. The other 8% contained these variances:
Wrong rates
Ghost (terminated, but still billed) employees
Employees with missing coverage
This is what slips through:
Paying for people who left
Terminated employees stay on carrier invoices. Without follow-up, premiums keep billing month after month.
Rates don’t match
Wrong rates, incorrect tiers, plan assignment errors – unflagged because no one is comparing invoice lines to the HRIS.
Enrollment never reached the carrier
Enrolled in the HRIS but the carrier has no record. Nobody catches it until a claim is denied.
Refunds missed
Carriers typically allow 30–60 days to recover overpayments. Miss that window and the money is gone.
Tabulera’s EDI Connectivity
From enrollment data to carrier-ready 834 files – Tabulera’s PEO solution handles the entire EDI pipeline.

Carrier Feed Setup & Maintenance
Tabulera handles it. Your team doesn’t have to.
- Go live in ~4 weeks, not 6 months
- Ongoing maintenance and spec updates included
- Carrier coordination and testing fully managed
Multi-Source Data Aggregation
Multiple HRIS platforms. One accurate carrier feed.
- Combine benefits enrollment and payroll from any source
- Start small. Scale without limits.
- No added headcount needed
Transmission
Visibility
Know exactly what was sent and what came back.
- Real-time status for every file
- Look up any member’s enrollment data instantly
- Full transaction history without touching raw EDI files
Why Getting EDI Carrier Feeds Live Takes Too Long
Most EDI vendors take six months. Internal teams aren’t faster. They’re buried in maintenance. New feeds? Back of the line.
The consequences stack up:
Feeds delayed. Enrollment by hand
Delayed feeds mean manual updates, coverage gaps, and stale data at the carrier. The backlog never clears.
Stuck maintaining
Spec changes, plan updates, carrier rejections – your team spends their time keeping old feeds alive instead of launching new ones.
Vendors keep failing
Slow turnaround. Poor communication. Missed deadlines. You switch vendors. Cycle starts over.
Workarounds become permanent
Feeds aren’t live, so someone manually updates carrier portals. That workaround quietly becomes the process.
Case Studies
Explore the outcomes employers and outsourcers achieve using Tabulera’s Benefits Reconciliation Software.
50,000 Lives and Every Acquisition Needed Carrier Feeds Yesterday.
Vensure needed carrier feeds live before new acquisitions could operate. Tabulera’s EDI made that possible in weeks – sometimes days.

CIO/COO
Vensure Employer Services
ZampHR Improves Monthly Reconciliation Efficiency by 75%
See how ZampHR (Engage PEO Company) streamlined benefits reconciliation for 13,000 employees, reconciling 130 monthly carrier invoices.

Director of Benefits
ZampHR
Why PEOs Choose Tabulera
Tabulera replaces the patchwork of spreadsheets, portal logins, and manual workarounds with a single platform built specifically for PEO benefits operations.
Replace spreadsheets
Automated matching catches billing errors that PEO HR software and manual audits miss.
EDI that actually ships
Carrier feeds go live in 30 days. Tabulera handles coordination, testing, and ongoing maintenance.
Works with your stack
PrismHR and isolved Marketplace partner. Both modules work with ANY HRIS, payroll or COBRA system.
Audit-ready
Full audit trails, issue tracking, and reconciliation reports. Every action documented.
Exceptional security
SOC-compliant infrastructure. Your data encrypted and securely maintained for PEO operations.
Fast to implement
Most PEOs are live within weeks. No long onboarding cycles. No six-month projects.
Use Cases for Tabulera's PEO Software
Whether you’re improving what’s broken or scaling what works – here’s what typically triggers the switch.
Exceptional security
Current vendor is slow, unresponsive, or losing files. You need someonewho actually ships.
Reducing Write-Offs
Write-offs keep growing. Finance wants answers. You need a system that catches variances before they hit the books.
Supporting Growth
More clients means more carriers and more invoices. Tabulera scaleswith you – same process whether you’re reconciling for 5 clients or 50.
How much are you writing-off?
Use our calculator to estimate potential leakage
What Makes Tabulera One of the Best PEO Software Solutions?
PEO Roots
Our founding team spent decades inside the Professional Employer Organization industry – running the same back-office workflows we now automate. Built for the complexity generic PEO technology solutions can’t handle.
PEOs' First Choice
Leading Professional Employer Organizations trust Tabulera to reconcile carrier invoices at scale – hundreds of clients, thousands of employees, dozens of carriers. No one else comes close.
Always Improving
SOC-compliant infrastructure. Regular platform updates. New features shipped based on what PEOs actually ask for — not a roadmap nobody sees. 200+ carrier connectors and growing.
PEO Software built to Integrate with Your Existing Systems
Marketplace partner – reconcile invoices and send EDI feeds using your PrismHR data directly.
Marketplace partner – pull enrollment and payroll data from isolved for reconciliation and EDI feeds.
Get Started with Tabulera’s PEO Software Today
“Tabulera’s Benefits Reconciliation Module has proven to be an invaluable tool, providing a scalable solution that meets the needs of a large PEO.”

Director of Benefits
ZampHR (an EngagePeo company)
FAQ
Why do ween need Tabulera’s PEO Software, when our platform already does “benefits administration”?
Founders of Tabulera spent more than 20 years in the PEO industry. The back-office benefit processes supported by Tabulera’s software have been historically unsupported by technology vendors. Professional Employer Organizations, however, are no exception. These processes are typically unsupported by any HRIS or accounting software. We call it full-cycle benefits premium administration.
How does Tabulera reconcile benefit invoices?
What is EDI connectivity in PEO software?
EDI connectivity means your enrollment data moves electronically between your PEO and insurance carriers using the 834 file format – no manual exports, no re-keying. Tabulera handles the carrier coordination, mapping, testing, and ongoing maintenance. Your team gets full visibility without carrying the operational weight.
